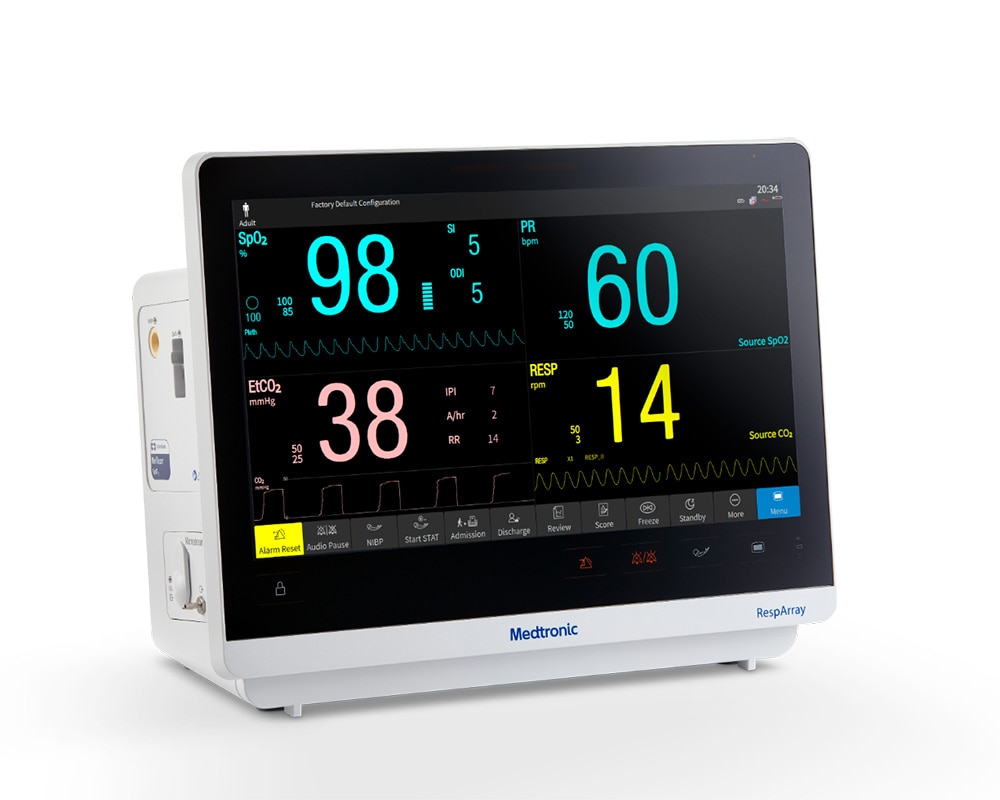
Intuitive Multiparameter Patient Monitoring
Patient safety made simple
97%1 of postoperative opioid-induced respiratory depression is likely preventable with better continuous monitoring and response.
Staffing shortages can make it challenging to check on your patients as often as you’d like.
But what if you could monitor patients from anywhere in the hospital? Now you can, with RespArray™, your multiparameter patient monitor.
It’s designed for areas of care where spot checking might not be enough, like in medical-surgical units, or where additional parameters are needed, such as capnography in procedural sedation. Helping you detect respiratory compromise early and intervene sooner. 2,3,4